Power personalized end-to-end experiences at scale
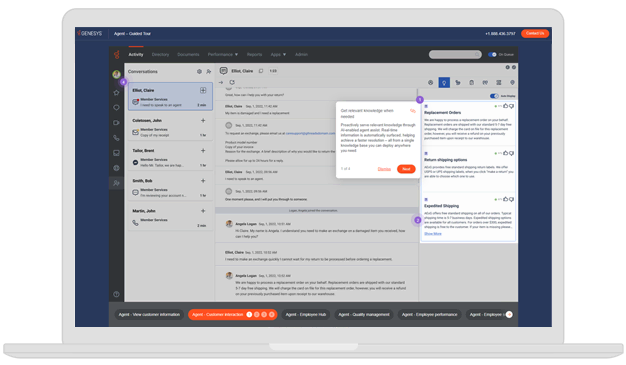
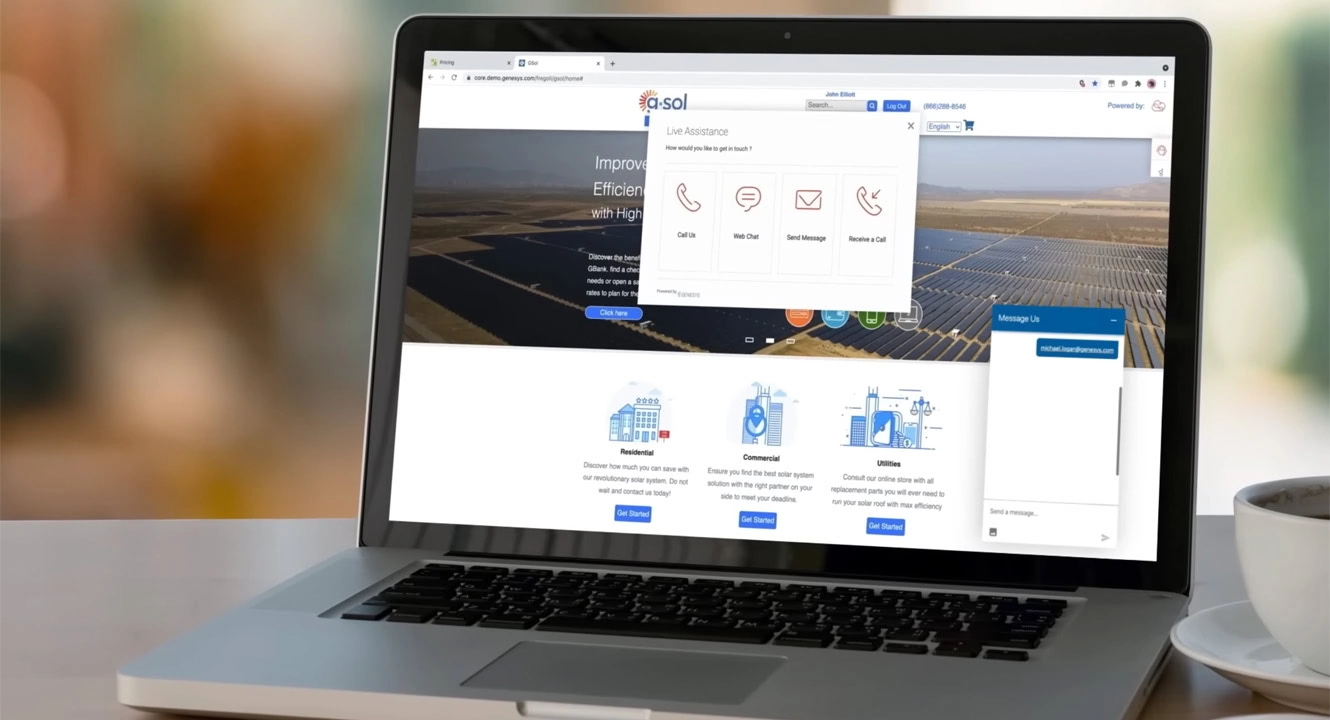
Genesys Cloud CX® is a leading AI‑Powered Experience Orchestration offering. With it, you can coordinate every step of your customer and employee experience by shaping journeys for moments that matter.
Trusted by businesses of all sizes in over 100 countries, Genesys Cloud CX is a leading customer and employee experience solution. It enables you to increase customer loyalty and employee retention with AI everywhere powering omnichannel engagements, intelligent routing, built-in workforce engagement, end-to-end journey management and more. Use one platform to power more connected, meaningful experiences. Every customer. Every interaction. Every time.